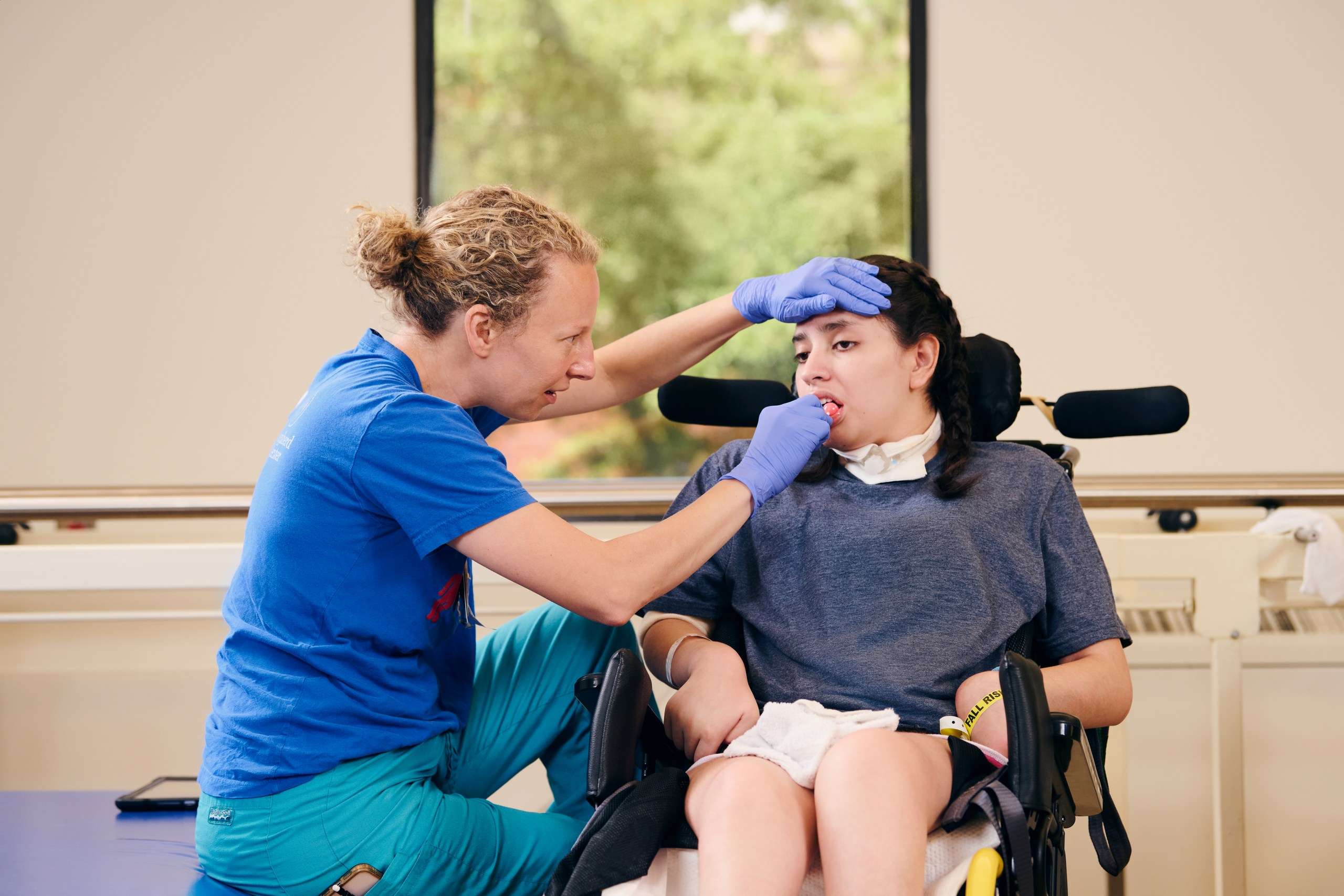
The Disorders of Consciousness (DoC) Program at Shepherd Center provides specialized services for individuals in a minimally conscious or reduced consciousness state due to a severe brain injury. Since 2000, our program has been one of only a few dedicated programs nationwide to meet the needs of these patients.
What is a disorder of consciousness?
Consciousness is defined as wakefulness or alertness with awareness of one’s self and the environment. Severe brain injuries can result in a disorder of consciousness, leading to reduced arousal and abnormal or limited reactions to environmental stimuli. Disorders of Consciousness include conditions such as coma, unresponsive wakefulness syndrome, and minimally conscious state, which significantly impact a patient’s ability to respond and interact.