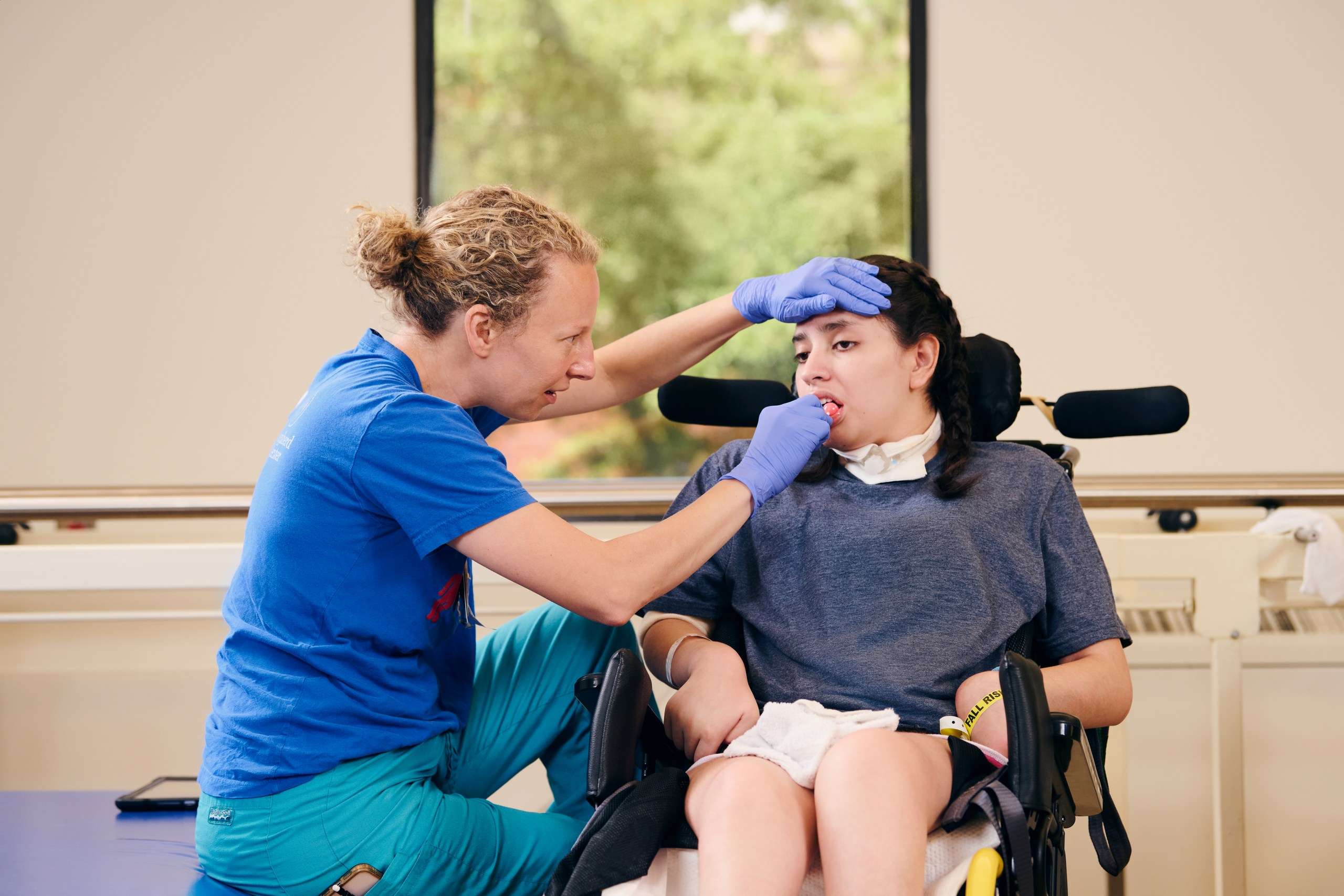
Specialized rehabilitation for coma, unresponsive wakefulness, and minimally conscious states after severe brain injury
The Disorders of Consciousness (DoC) Program at Shepherd Center offers highly personalized, evidence‑based rehabilitation for individuals in a minimally conscious or reduced‑consciousness state after a severe brain injury. For more than two decades, we’ve been one of the few specialized DoC programs in the country dedicated to supporting patients and families during this deeply challenging time.
Program overview
Our Disorders of Consciousness Program is designed for individuals who require specialized neurological care beyond traditional inpatient rehabilitation. This phase of disorders of consciousness rehabilitation focuses on medical stability, arousal, responsiveness, and preparation for the next level of recovery.
Your loved one may participate in a structured minimal conscious state rehabilitation approach that combines sensory stimulation, positioning, communication trials, and early functional activities based on their neurological presentation.
Who we treat
We care for adolescents and adults with severe acquired brain injury (traumatic or non‑traumatic) who are medically stable and present with reduced or minimally conscious states. Typical indicators include a present sleep/wake cycle, inconsistent or absent command following, and the need for structured arousal and communication trials. Final eligibility is determined by our interdisciplinary team after clinical review.